This means that osteoblasts act as mediators between thyroid hormone and osteoclasts the cells that tear down bone. My Endocrinologist has been treating me for both with synthroid as well as Fosomax.
 Thyroid Disorders Can Raise Risk For Osteoporosis And Spinal Fracture
Thyroid Disorders Can Raise Risk For Osteoporosis And Spinal Fracture
Hypothyroidismlow thyroid functionclearly causes impaired bone formation in children.

Thyroid and bone density. The nodules have grown and the bone density has decreased. A normal thyroid gland produces 6 mcg of T3 daily so this lack of direct T3 over time could contribute to osteopeniaosteoporosis. Your doctor will assess your need for a bone density scan based on your risk factors and refer you for a scan if necessary.
In adults the effects of hypothyroidism are less clear but over time could also lead to weaker bones. Subclinical thyroid dysfunction in which the TSH is abnormal but the T4 and T3 levels are normal is common in the elderly but its relationship to bone mineral density and hip fracture in this population remains unclear. It may well be that since lowered bone density and hypothyroidism occur naturally at the same life stage during menopause and andropause for women and men respectively the two conditions may have been incorrectly correlated by researchers.
This is called hyperparathyroid disease or hyperparathyroidism. Only when patients have had actual Graves disease overactive thyroid is there a risk of osteoporosis and even that risk is small. The parathyroid can cause osteoporosis by making too much PTH which eventually makes your body take calcium from your bones.
Hyperthyroidisman overactive thyroidcan accelerate bone breakdown and cause osteoporosisliterally weak porous bones. This loss is documented by the measurement of bone density densitometry and leads to an increased risk of broken bones fractures. Decreased bone density and osteoporosis.
Linking Thyroid Disorders and Bone Loss Thyroid disorders are considered secondary causes of osteoporosis. Hyperthyroidism and Bone Health. Osteoporosis is more common in women with Hashimotos and thyroid conditions who take thyroid medications as thyroid hormones speed up bone turnover.
Hyperthyroidism is associated with an increased excretion of calcium and phosphorous in the urine and stool which results in a loss of bone mineral. Hyperthyroidism together with other risk factors for osteoporosis. Without sufficient T3 then normal bone remodeling is disrupted and bone resorption happens at a more rapid rate than bone building.
This loss is documented by the measurement of bone density densitometry and leads to an increased risk of broken bones fractures. An overactive thyroid hyperthyroidism can increase the chance of getting osteoporosis. Hyperthyroidism is associated with an increased excretion of calcium and phosphorous in the urine and stool which results in a loss of bone mineral.
If someone is doing well on thyroid hormone but the dosage is so high that it is affecting the patients bone density then it makes sense to try to find the underlying cause of the condition so that the person might not have to take thyroid hormone daily forever. That means thyroid disorders do not directly cause osteoporosis or spinal fractures but abnormal levels of thyroid hormone may influence your bodys metabolismits ability to maintain healthy bone density through the remodeling process. I have begun taking a daily injection of Forteo for my bone loss.
Treatment of thyroid overactivity will reduce the rate of bone loss and bone strength may. Studies have shown NO reduction in bone mineral density and no osteoporosis when thyroxine is taken even in suppressive doses. Underactive thyroid hypothyroidism An underactive thyroid is not in itself a risk factor for osteoporosis but if you are prescribed levothyroxine to increase your thyroid levels to the normal range you should have regular blood tests at least once a year to ensure your thyroid hormone levels are not too high.
The simple rule therefore is to test your blood thyroid hormone levels every 6 months. These changes in bone metabolism are associated with negative calcium balance high calcium levels in the urine and rarely high serum calcium levels 15. If a bone density scan shows osteoporosis then this can be treated with medication.
Talk to your doctor about a bone mineral density scan if you have had prolonged untreated. Several previous studies examining the effects of subclinical thyroid dysfunction on bone have had mixed results. Reuters Health - Thyroid surgery that totally or partially removes the gland may increase the long-term risk of bone thinning and bone breaks especially for younger patients and women according.
Once your thyroid problem is controlled bone density usually recovers. I have had problems with nodules on my thyroid for the past 3 years as well as low bone density. Overt hyperthyroidism is associated with accelerated bone remodeling reduced bone density osteoporosis and an increase in fracture rate 15.
In pharmacy school I learned that osteoporosis was a progressive condition that could be slowed down but never really reversed. Hyperthyroidism is one of a number of conditions that can cause a reduction in bone density. There are anecdotal reports on thyroid internet forums where women switching from T4 to desiccated thyroid have reported improved bone density.
This once again is where natural thyroid treatments might be beneficial.
This doesnt necessarily mean theres permanent damage to the nerve that controls the vocal cords. Gastric bypass surgery is a very dangerous surgery.
Thyroid Surgery Or Thyroidectomy Dr Vivian C Simmons
The average blood loss for thyroid operations is usually small and the chance of needing a blood transfusion is extremely rare.
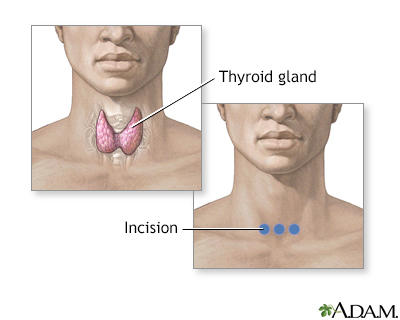
How dangerous is thyroid surgery. This drain is usually removed the morning after surgery. Thyroid operations that a surgeon may perform are of various kinds including. Although the surgery is usually safe there are risks like bleeding damage to the nerves.
Complications are uncommon but the most serious possible risks of thyroid surgery include. 8 2019 HealthDay News -- Surgery to remove all or part of the thyroid can trigger side effects that send some patients back to the hospital a new study finds. Temporary or permanent hoarseness or loss of voice.
It may also occur if the nerves to the larynx or vocal cords are damaged during surgery. Overall thyroid surgery isnt considered dangerous. The parathyroid glands are located near the thyroid gland and may be injured during thyroid surgery.
What thyroid hormones are. Other risks include heavy bleeding and infection. Literature review on the outcome and safety of thyroid surgery in elderly patients has been filled with conflicting results and this subject remains controversial.
Well it depends on your surgery typea partial or complete removal of the thyroid. 1 Complications are much less common and can include bleeding a neck hematoma permanent. Potential complications of thyroid surgery include.
However the relative risk of complications is very low and is usually outweighed by the potential benefits of having the surgery. And if you do some of your own research youll see that complications from thyroid surgery arent too uncommon. Some people may need to have a drain placed under the incision in the neck.
Side effects of surgery are common and include neck pain a sore throat difficulty swallowing hoarseness and temporary hypoparathyroidism. This can happen if the larynx voice box or windpipe is irritated by the breathing tube that was used during surgery. The surgery is performed under general anesthesia.
Thyroid surgery can cause damage to the laryngeal nerve as well as the parathyroid glands. There is also a small risk associated with anesthesia. The main risks of thyroid surgery include.
How Long Does Thyroid Surgery Take. This can result in a drop in blood calcium levels. One of the main parts of thyroid cancer treatment is removing all or part of the thyroid gland.
As with any operation there is always a chance of bleeding. A variety of thyroid conditions have thyroid surgery as the answer including cancerous and non cancerous thyroid nodules overactive thyroid glands and large thyroid glands goiters. Tingling in the fingers that can progress to tremors Spasms in all muscles of the body including the heart and muscles surrounding the lungs Low calcium levels hypocalcemia.
In experienced hands thyroid surgery is generally very safe. Other side effects of thyroid removal surgery thyroidectomy that may require patients to be re-hospitalized include. After thyroidectomy a few people may experience neck pain and a hoarse or weak voice.
If you are having thyroid surgery known as a thyroidectomy its important to know what to expect as you recover. A person has an overactive. Bleeding in the hours right after surgery that could lead to acute respiratory distress.
An increasing elderly population a rising incidence of differentiated thyroid carcinoma DTC and a rising incidence of benign nodular disease with age are all contributing to a rise in thyroid operations for the elderly. A thyroid nodule or the whole gland is enlarged and causing dangerous or bothersome symptoms such as trouble swallowing difficulty breathing or changes to the voice. Risks of thyroid surgery As with every major surgery thyroid surgery carries the risk of an adverse reaction to general anesthetic.
Due to these risks thyroid surgery should usually be a last resort after every other option has failed. Bleeding in the neck. The issues surrounding thyroid disease in patients undergoing nonthyroid.
One night stay is required for complete thyroid removalwhile in partial thyroid lobectomy some hours of stay is enough. Most people will experience minor discomfort and short thyroid surgery recovery times and most will be back on their feet as soon as the next day after the surgery is complete with activity restrictions of course. Some side effects of a gastric bypass surgery are confusion nightmares sweating shaking headaches and many more.
So the question arises how much hospitalization time is required in this procedure. Although most patients with well-compensated thyroid disease do not need special consideration prior to surgery patients who have a newly diagnosed thyroid disorder around the time of surgery require a discussion of the risks and benefits of proceeding with surgery.
Symptoms can include swelling or a lump in the neck. Dabrafenib Tafinlar and trametinib Mekinist can be used to treat cancers with certain BRAF gene changes.
 Medullary Thyroid Carcinoma Beyond Surgery Advances Challenges And Perspectives In Endocrine Related Cancer Volume 26 Issue 9 2019
Medullary Thyroid Carcinoma Beyond Surgery Advances Challenges And Perspectives In Endocrine Related Cancer Volume 26 Issue 9 2019
Doctors usually recommend aggressive treatment to kill off the rogue cells and in some patients treatment is highly effective.

Metastatic medullary thyroid cancer treatment. Other patients may have less responsive cancers. According to a story from The ASCO Post the drug cabozantinib marketed as Cometriq was first approved by the US Food and Drug Administration FDA as a treatment for metastatic medullary thyroid cancer on November 29th 2012. Anlotinib for the Treatment of Patients with Locally Advanced or Metastatic Medullary Thyroid Cancer.
This often fatal disease had no approved treatments until 2011. Treatment options include resection or percutaneous radiofrequency ablation. Cancer can also occur in the thyroid after spread from other locations in which case it is not classified as thyroid cancer.
The primary treatment for medullary thyroid carcinoma MTC is extensive and meticulous surgical resection. Each year we treat between 175 and 350 medullary thyroid cancer MTC patients many of whom have progressive metastatic disease Although thyroid cancers tend to be slow growing those with progressive metastatic MTC face different odds. Clinical manifestations diagnosis and staging The primary treatment for MTC is extensive and meticulous surgical resection.
In certain people with a high risk for MTC such as people carrying certain gene changes a thyroidectomy may be performed to prevent cancer. Its difficult to predict how fast metastatic medullary thyroid cancer will progress. Thyroid cancer is cancer that develops from the tissues of the thyroid gland.
Advanced RET fusion-positive thyroid cancer requiring systemic therapy and RET fusion-positive nonsmall cell lung cancer. Targeted therapy with a tyrosine kinase inhibitor vandetanib cabozantinib or selpercatinib for cancer that has spread to other parts of the body. The prognosis for a patient with metastatic thyroid cancer depends on factors like the size of the metastases and their precise location.
MTC is usually treated by removing the thyroid. Treatment of locally advancedmetastatic medullary thyroid cancer may include the following. Though it isnt curable once it has metastasized palliative treatments such as targeted chemotherapy and.
Liver metastases occur in 45 of MTC patients with local or metastatic disease 6. MEN 2B consists of MTC pheochromocytoma in 50 of patients. You may be offered chemotherapy for locally advanced or metastatic medullary carcinoma if targeted therapy doesnt work.
Surgery and radiation therapy have been the major treatments for medullary thyroid carcinoma. Selpercatinib Retevmo can be used to treat cancers with certain RET gene changes. Get detailed information about the treatment options for newly diagnosed and recurrent thyroid cancer in this summary for clinicians.
There is a limited role for external beam radiotherapy. Thyroid cancer treatments include surgery radiation therapy radioactive iodine therapy chemotherapy hormone therapy targeted therapy and observation. See Medullary thyroid cancer.
In large progressive liver metastases or metastases associated with symptoms local treatment is required. Thyroid hormone therapy is not as effective as surgical treatment for MTCs which are. Make sure you have a true medullary thyroid cancer surgery expert.
In fact in favorable smaller medullary thyroid cancers surgery is not only the first treatment but is commonly the only treatment that may be indicated. It is usually given as a palliative treatment to help relieve symptoms. MEN 2A Sipple syndrome consists of MTC pheochromocytoma in 50 of patients and hyperparathyroidism 10-20 of patients.
A second therapy was approved by the Food and Drug Administration FDA in November 2012. Besides surgery sometimes other treatments are also required including radiation therapy or chemotherapy. A plasma level of metanephrines should be checked before surgical thyroidectomy takes place to evaluate for the presence of pheochromocytoma since 25 of people found to have medullary thyroid cancer have the inherited form from the MEN2A syndrome.
MD Anderson played a key role in the development of both treatments. Larotrectinib Vitrakvi or entrectinib Rozlytrek can be used to treat cancers with NTRK gene changes. For medullary thyroid cancer surgery by far is the most common first treatment.
Anlotinib demonstrated a durable antitumor activity with a manageable adverse event profile in locally advanced or metastatic MTC. Herein we report a case of a patient with initially unresectable widely metastatic RET-mutated medullary thyroid carcinoma treated on a single-patient clinical pro-tocol with neoadjuvant selpercatinibLOXO-292 followed. This surgery is called a thyroidectomy.
Chemotherapy drugs used for medullary carcinoma include doxorubicin Adriamycin and dacarbazine DTIC. It is a disease in which cells grow abnormally and have the potential to spread to other parts of the body. As this drug was approved for progressive metastatic disease meaning disease that has spread to other tissues beyond its area of origin the treatment is typically.
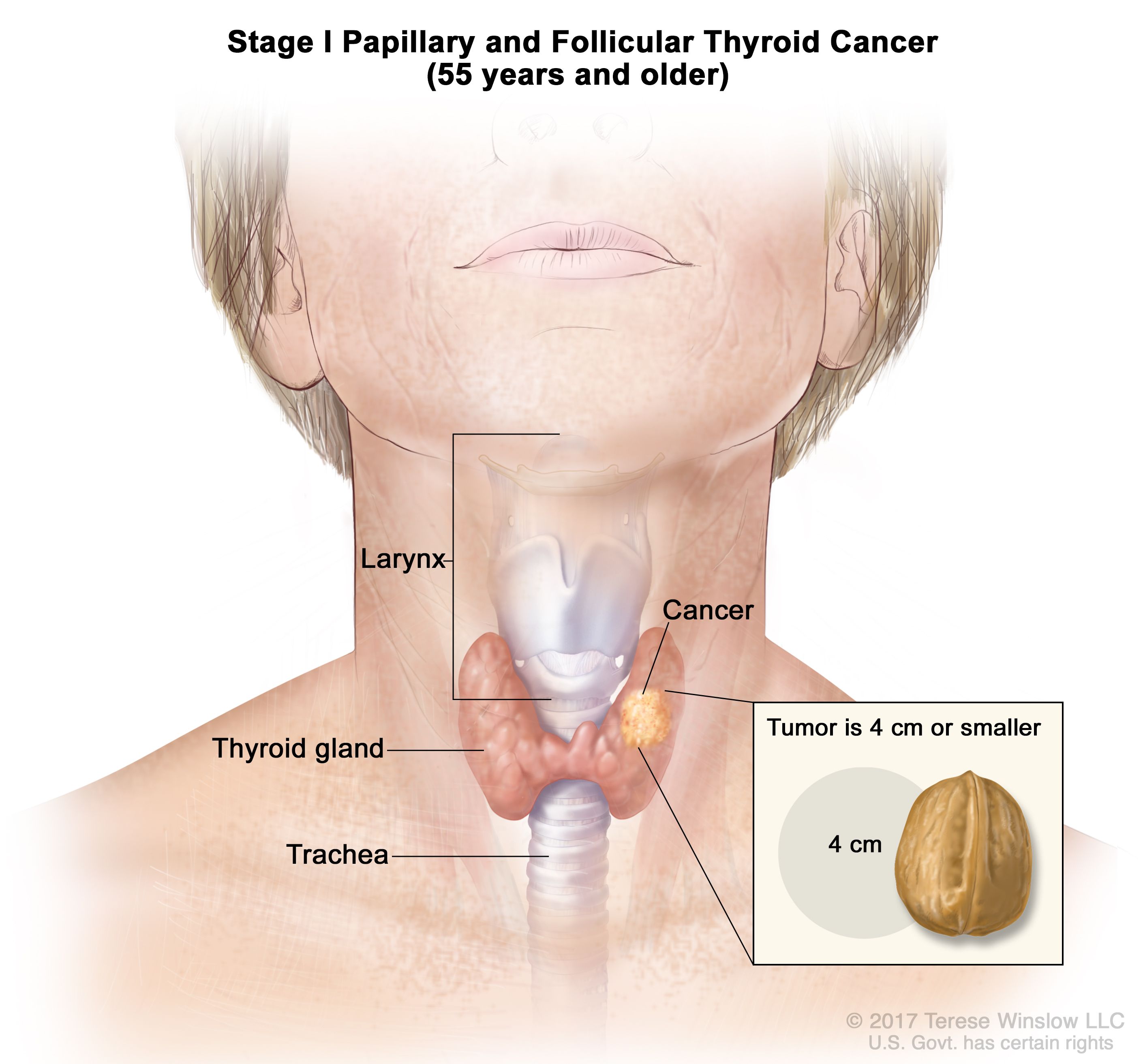
If the cancer has spread lymph nodes in the neck area may. Thyroid nodules are solid or fluid-filled lumps or bumps.
 Endocrine Surgery Thyroid Cancer
Endocrine Surgery Thyroid Cancer
If thyroid cancer is diagnosed by a fine needle aspiration FNA biopsy surgery to remove the tumor and all or part of the remaining thyroid gland is usually recommended.

Growth on thyroid gland surgery. The incision causes pain for a day or two after surgery and it leaves a scar which is usually relatively inapparent after a year. Once again sometimes they will surgically remove part or all of the thyroid gland and not just the nodule or cyst. Several conditions can cause nodules to develop in your thyroid gland including.
The thyroid is part of the endocrine system which is made up of glands that secrete various hormones into the bloodstream. The gland is shaped like a butterfly and wraps around the windpipe or trachea. You can ask your surgeon about this prior to your surgery.
The term thyroid nodule refers to any abnormal growth that forms a lump in the thyroid gland. A thyroidectomy is when all or part of the thyroid gland is removed. Lobectomy A lobectomy is an operation that removes the lobe containing the cancer usually along with the isthmus the small piece of the gland that acts as a bridge between the left and right lobes.
Thyroid surgery can also cure certain forms of thyroid gland overactivity associated with goiter or nodules. Near Total Thyroidectomy NTT is associated with a low rate of recurrence. An overgrowth of normal thyroid tissue is sometimes referred to as a thyroid adenoma.
Half of the thyroid gland. Evaluation and Preparation for Surgery. A common treatment for cancerous nodules is surgical removal.
A lobectomy is when one of the two lobes of your thyroid is removed. Its unclear why this occurs but its not cancerous and isnt considered serious unless it causes bothersome symptoms from its size. Both operations are generally carried out under general anaesthesia.
Thyroid Cancer Surgery for Central Compartment Lymph Nodes. Subtotal Thyroidectomy ST in which a portion of the thyroid gland is deliberately left in the thyroid lodge has a considerably higher rate of recurrence. When the calcium level is low in your bloodstream these glands release parathyroid hormone PTH which takes calcium from your bones.
Parathyroid gland removal refers to a type of surgery done to. Thyroid nodules are usually. Even a benign growth on your thyroid gland can cause symptoms.
A thyroid nodule may require surgical removal. If a thyroid nodule is causing voice or swallowing problems your doctor may recommend treating it with surgery to remove all or part of the thyroid gland. The incidence of complications with TT is similar to that with other techniques of thyroid exeresis.
These antibodies inflame the thyroid causing hormone overproduction. In the past it was standard to remove a majority of thyroid tissue a procedure called near-total thyroidectomy. If the doctor recommends removal of your thyroid thyroidectomy you may not even have to worry about a scar on your neck.
A total thyroidectomy is an operation to remove all of thyroid gland. The removal of the lymph nodes of the central neck can be performed initially when the thyroid gland is removed in the treatment of the thyroid cancer or following the initial surgery in the less common circumstances when thyroid cancer recurs or persists. Overgrowth of normal thyroid tissue.
A nodule on the gland is cancerous or may become cancerous. However today more limited surgery to remove only half of the thyroid may be appropriate for some cancerous nodules. A thyroid nodule is an unusual growth lump of thyroid cells in the thyroid gland.
If the thyroid nodule or cyst is causing difficulty breathing andor swallowing then this is yet another reason why surgery might be required. A 2018 study found that giving potassium iodide during thyroid surgery was associated with less transient hypoparathyroidism and hoarseness and may improve the safety of the procedure for those with Graves disease. The thyroid is a butterfly-shaped organ or gland that is located on the front of the neck just under the Adams apple larynx.
A thyroid lobectomy or hemi thyroidectomy is to remove one lobe ie. Theyre found on your thyroid a small powerful gland in your neckThis gland makes thyroid hormone which affects your metabolism the. There are several kinds of thyroid surgery which are taken as an option for treatment but the most common among them are as follows-Lobectomy is a kind of thyroid adenoma surgery which we undergo when half of the thyroid gland gets adversely affected by infectious tissues.
The thyroid gland is located low in the front of the neck below the Adams apple. Thyroid surgery almost always requires hospitalization and anesthesia. Graves disease causes the body to misidentify the thyroid gland as a foreign body and send antibodies to attack it.
A person is most likely to undergo thyroid removal surgery if.